In March 2011, when Larry Merlo became CEO of CVS Caremark Corp., he inherited some aches and pains. Four years earlier U.S. drugstore operator CVS had made a bold bet with its $26.5 billion acquisition of Caremark Rx, a pharmacy benefit manager (PBM) that serves as an intermediary between pharmaceuticals companies and groups that pay for drugs, like insurance companies and corporations. By the time Merlo took over the top job from longtime CEO Thomas Ryan, the deal was looking like a bust, and some analysts were calling for CVS to spin off its Caremark business.
The new chief executive, who began his career in 1977 as a pharmacist and assistant manager with Peoples Drug Stores (later bought by CVS), responded firmly. He stressed on an earnings call his confidence that the company had “the right assets in place to ensure our long-term success in this changing health care environment.”
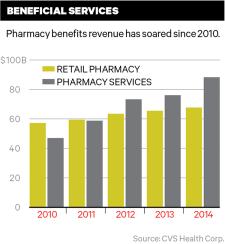
Today, Merlo, 59, spends much less time defending his vision for his company, which was renamed CVS Health Corp. in 2014 to reflect its broad ambitions. The results speak for themselves. Shares have climbed steadily, from $33 in March 2011 to $107 in mid-August of this year — a 224 percent improvement over Merlo’s tenure. Annual revenue has followed a similar trajectory, hitting a record $139 billion at the end of 2014, up nearly 30 percent since 2011. While CVS’s retail segment has boasted gains — posting revenue of $67.8 billion in 2014, a 14 percent increase over 2011 — it’s the PBM business that has really thrived: Its revenue grew to $88.4 billion in 2014, up 50 percent under Merlo.
“The surprise with Larry is no one thought of him as a strategic guy, but he’s clearly taken what he got and made it even more unique through acquisitions and building out the vertical model,” says Scott Mushkin, senior retail and consumer staples analyst at Wolfe Research in New York. “CVS has an incredibly unique business model. They’re the only fully integrated retail, health care, pharmacy benefit manager specialty company out there.”
The transformation of Woonsocket, Rhode Island–based CVS from a drugstore chain into a new kind of health care company began under former CEO Ryan. In 2004, CVS bought Eckerd Stores and Eckerd Health Services, which included a $1 billion mail order and PBM business. In 2006 it acquired MinuteClinic, the largest provider of retail health care in the U.S.
Merlo has placed his own stamp on CVS’s ongoing metamorphosis. In January 2014, CVS paid $2.1 billion for Coram, gaining a foothold in the infusion and enteral nutrition services business. This May it doled out $12.7 billion for Omnicare, which supplies prescription medicine to nursing and assisted-living homes. The very next month CVS announced it would pay $1.9 billion for more than 1,600 of Target Corp.’s pharmacies and 80 of the discount retailer’s walk-in clinics.
Merlo, who grew up in a small working-class town in Pennsylvania and has a pharmacy degree from the University of Pittsburgh, says his vision for CVS was formed in part by his early career as a pharmacist. Last year CVS completed the rollout of Specialty Connect, which integrates its specialty pharmacy and retail businesses to provide members with disease-state-specific counseling from pharmacists. The company’s Pharmacy Advisor program alerts pharmacists when patients are not adhering to their medication regimens. “There’s even more that pharmacists can do to practice at the top of their license,” Merlo says. “I think we have an opportunity across the country to recognize the skill and the intensity of their education.”
Institutional Investor Senior Contributing Writer Katie Gilbert recently spoke with Merlo about his vision for CVS and why moves like the company’s decision last year to halt sales of tobacco products are integral to its success.
Institutional Investor: What is the significance of changing the company’s name to CVS Health Corp.?
Merlo: The change of the company name to CVS Health really reflects the purpose we have as an organization of helping people on their path to better health, along with our broader health care commitment. We see CVS Health changing the way health care is delivered. We have three goals in mind: We have the ability to increase access to care, to lower the overall cost of care and at the same time to improve the quality of care in helping to improve outcomes.
Each year, through our integrated business model, we touch more than 100 million people by playing an active or supportive role in each person’s health experience. Obviously, that’s impacting the greater health care environment. We’ve demonstrated an ability to deliver breakthrough products and services that we think are helping businesses — whether it’s an employer client or a health plan — and their members and the communities in which they live to help manage health in more affordable, effective ways.
Can you provide some examples?
The statistics around medication adherence — people staying on the prescriptions that are prescribed — are pretty alarming. Three out of four people, within one year of being diagnosed with a chronic disease, are not taking meds as prescribed. We think of that as an epidemic. Studies on this quantify the impact on health care approaching $300 billion a year in unnecessary and avoidable costs. The products and services we’ve been bringing into the market have been proven to improve medication adherence, with an appropriate return on investment for plan sponsors.
Then you think about the role that our MinuteClinics play. Today we have about 1,000 of those clinics. We look at our own employee population as a learning lab. One of the things we looked at a few years back is which of our employees had access to and utilized a MinuteClinic. When we adjusted for age and health status to create an accurate and statistically valid comparison, we found that those employees [who visited MinuteClinics] had 8 percent lower overall health care costs. A piece of that was getting visits outside of the emergency room. Fifty percent of the patients that we see across the country in MinuteClinics are seen during the evening hours and on weekends, often when their physician isn’t available.
Does the rise of health care consumerism have anything to do with the Affordable Care Act?
We’ve coined the term “retailization of health care.” In part that’s being driven by the increasing number of individuals that are in consumer-driven health plans. We see consumers playing an increasingly active role in health care decisions. I think the growth of private exchanges and the emergence of the public exchanges are putting the decision of health plan choice directly into the hands of the consumer. The growth of these consumer-directed plans is driving consumers to be more involved and take more fiscal accountability for their health care choices.
At the same time, that also requires the consumer to be provided the appropriate level of education and the tools to help them make informed decisions. Again, I think our unique business model plays an important role when you think about the accessibility of the pharmacist. The pharmacist continues to be one of the most trusted health care professionals, according to surveys.
CVS has announced plans to operate 1,500 MinuteClinics within two years, despite the fact that they aren’t very profitable. Why is this an important goal?
We continue to have an opportunity to broaden and expand the scope of services that we provide. When MinuteClinic was born, so to speak, it was focused only on acute conditions, and we have been doing more to manage chronic disease, recognizing that today 50 percent of all Americans suffer from one or more chronic diseases.
With the Affordable Care Act, we have millions of newly insured Americans seeking care. When you think about the fact that today there is a shortage of primary care physicians, those factors are going to place additional stress on our health care delivery system. This shortage is expected to approach 50,000 by the end of this decade. So we see MinuteClinic having an opportunity to play a growing role in the delivery system.
Where is the profit opportunity in MinuteClinic given its low margins?
I do think MinuteClinic has played a role in helping us win new PBM business. We’ve been public about the fact that MinuteClinic operates at a break-even level on what we describe as an enterprise basis.
We’re a large employer ourselves, and there are PBM clients that share the same goals in terms of making sure they’re providing access to care for their employees in the most cost-effective way, without putting the cost simply on the backs of one’s respective employees.
Has the consolidation among pharmacy benefit manager providers limited CVS’s ability to grow and expand?
Obviously, there’s a lot that’s changing in the marketplace. But we certainly continue to see opportunities for growth. We view health plans as a very important growth opportunity, and we view the consolidation in that sector as a positive factor for realizing that growth. The marketplace has been competitive in pharmacy for years. We think that will continue. We don’t see this consolidation changing that dynamic.
Could CVS play a role in helping to lower the cost of drugs for consumers?
We’ve got quantifiable data that shows that we’ve been able to reduce pharmacy costs for plan sponsors and their members in a variety of ways. One way we’ve been able to do that is through our unique formulary management system, which includes products like Maintenance Choice. That product gives members the option of choosing mail pharmacy or CVS retail pharmacy, and it preserves the cost savings economics for both the plan sponsor and the members.
How is the company positioning itself to benefit as the U.S. population ages?
The Omnicare acquisition will significantly expand our customer reach to a broader population. We did not serve that patient segment, when you think about pharmacy services to long-term care.
In the U.S. there are 10,000 baby boomers who are turning 65 and becoming Medicare-eligible every day, and that trend is going to continue for more than a decade. More people are projected to use assisted-living facilities and independent-living communities. We see that as a substantial growth opportunity, as we can provide innovative solutions to serve that patient population.
Was the decision to stop selling tobacco products an important move as you position CVS as a fit partner for health insurers, physician groups and others?
It’s been more than a year now since we announced the decision in February 2014. The contradiction of selling tobacco in the same four walls where health care was being delivered — that contradiction has been out there for many years. There’s a big difference between being a drugstore and a health care company. We see, now more than ever, pharmacies are extending the front lines of care, becoming more involved in chronic disease management. I mentioned earlier that we’ve got 50 percent of all Americans suffering from one or more chronic conditions, whether it’s hypertension or high cholesterol or diabetes. All of those conditions are made worse by smoking. While it was not an easy decision financially, we said: “It is the right thing to do. It is a barrier to the future growth of the company, and cigarettes have no place in a setting where health care is being delivered.”
There’s no question that [the decision to stop selling tobacco products] has opened up new partnerships. Today we have more than 60 clinical affiliations, with some nationally recognized institutions, like Cleveland Clinic, Dartmouth-Hitchcock, UCLA Health, the Henry Ford Health System and Emory Healthcare.
At the same time, it’s hard to sit here and say, “We won a new PBM client because we stopped selling tobacco.” I can’t say that, but I think it’s more than an intangible when you’re sitting across the table from a prospective client and talking about the things that we can do and the products and services that we provide and that we view ourselves as a health care organization — a pharmacy innovation company. I think it has brought credibility to our marketing story and our message. •
Get more on corporations.





